Mastitis, Clogged Ducts & Engorgement: An IBCLC's Complete Guide
By Jennifer Chivas, RN BSN IBCLC — Lactation Loop
If you've woken up with a rock-hard, red, burning breast and a fever that came out of nowhere, you already know how fast mastitis can knock you off your feet. It feels like the flu and a breast infection arrived at the same time — because that's essentially what's happening.
Mastitis is one of the most common reasons breastfeeding moms call us in a panic, and it's also one of the most misunderstood. Moms often confuse it with a clogged duct (understandable — the early stages look similar), try to push through without treatment, or do things that accidentally make it worse.
This guide walks you through engorgement, clogged ducts, and mastitis — what each one is, how to tell them apart, how to treat them at home, and exactly when to call your doctor or IBCLC. Written by our board-certified IBCLCs who work with breastfeeding families every day across Florida, Michigan, Texas, New York, North Carolina, and Indiana.
What Is Mastitis?
Mastitis is inflammation of the breast tissue. It can be infectious (caused by bacteria) or non-infectious (caused by milk stasis — milk that isn't moving). Either way, it's painful, it comes on fast, and it needs to be taken seriously.
Mastitis affects approximately 10% of breastfeeding mothers in the U.S. — so if you're dealing with it, you're far from alone. It most commonly occurs in the first few weeks postpartum, but it can develop at any stage of breastfeeding.
Mastitis Symptoms: What to Look For
Mastitis typically presents on one side only. Symptoms include:
A hard, swollen, painful area in one breast — often wedge-shaped
Redness and warmth over the affected area
Fever of 101°F (38.5°C) or higher
Flu-like symptoms — body aches, chills, fatigue, feeling like you've been hit by a truck
Breast pain that doesn't improve after nursing or pumping
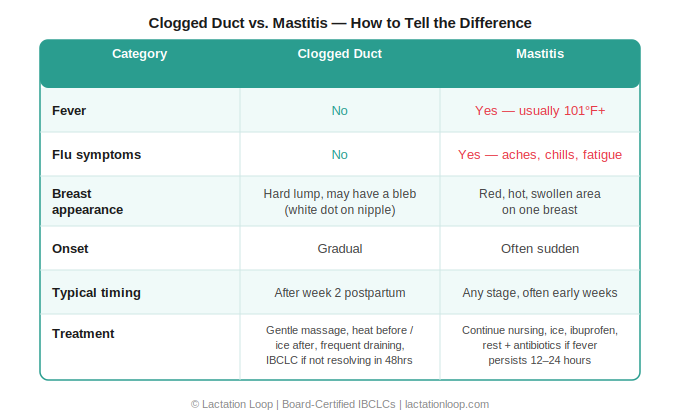
The fever and flu-like symptoms are the key distinguishing factor between mastitis and a clogged duct. If you feel sick all over — not just in your breast — that's mastitis until proven otherwise.
Mastitis With No Fever — Is It Still Mastitis?
Yes, it can be. In the early stages of mastitis, or in non-infectious mastitis, fever may not be present yet. If you have significant breast pain, redness, and hardness in one area but no fever, treat it as a developing mastitis and begin home management immediately. If symptoms don't improve within 12–24 hours, call your provider.
Engorgement: The Starting Point
Engorgement is a natural part of the postpartum process — it's not a problem, it's a sign your body is doing exactly what it's supposed to do. It typically happens in the first few days after birth and marks the beginning of milk production (lactogenesis).
Engorgement does not mean your breasts are full of milk. It means breast tissue is swelling hormonally to prepare for production. The breast has been activated and knows it has a job to do.
What helps:
Feed on demand — this is the single most effective treatment
Apply a warm compress for a few minutes before feeding to soften the tissue and help baby achieve a deeper latch
Hand express a small amount before latching if needed to soften the areola
Ice the breast for about 15 minutes after feeding if you're having severe discomfort — but don't overdo it, as too much ice can reduce supply
Ibuprofen for pain and inflammation (safe while breastfeeding at standard doses)
Avoid: stopping ibuprofen abruptly if you've been taking it — engorgement can flare quickly when the anti-inflammatory effect drops off.
Clogged Ducts: Causes, Signs & Treatment
Clogged ducts typically develop after week two postpartum, once milk production is fully established. They're localized to one specific area of the breast — unlike engorgement, which affects the whole breast.
Signs of a Clogged Duct
A hard, round lump in one spot that doesn't resolve after nursing
A bleb — a small white dot on the tip of the nipple (a blocked duct opening)
Reduced output on the affected side
Discomfort in a specific area — but no fever, no flu symptoms
What Causes Clogged Ducts?
The number one cause is interrupted or incomplete breast emptying. Common culprits include:
Shallow latch — baby isn't effectively draining the breast
Ill-fitting pump flange — milk isn't being fully expressed
Tight-fitting bra — compressing milk ducts
Skipped feedings — going too long between sessions
Mature, fattier milk — which moves more slowly
Milk cyst (galactocele) — a benign, fluid-filled cyst that can develop during lactation
How to Treat a Clogged Duct at Home
Gentle massage — start from the front of the clog (closest to the nipple) and work slowly backward. Never massage from the back forward — this can push milk into surrounding tissue and increase swelling.
Heat before, ice after — apply a warm compress for up to 15 minutes before nursing or pumping to encourage flow. After draining the area, ice for up to 15 minutes to reduce inflammation. Don't exceed 15 minutes on either end.
Drain frequently — offer the affected breast first at each feeding. Positioning baby so their chin points toward the clog can help target that area.
Hand expression — after nursing or pumping, hand express for 1–2 minutes, focusing on the clogged area, to clear any remaining backup.
If a clog isn't resolving within 24–48 hours despite these measures, reach out to an IBCLC. We can help identify the root cause and get things moving — sometimes in a single visit.
Mastitis Treatment: What to Do at Home
The most important thing to know about mastitis: keep the milk moving. Milk stasis (milk that isn't flowing) makes mastitis worse. Do not stop breastfeeding or pumping.
Step 1: Keep Draining the Breast
Continue nursing or pumping on a regular schedule — every 2–3 hours. During feeding or pumping, use hands-on pumping: gentle breast compression starting from the front of the affected area, working backward, to help move milk through. Do not add vibration or deep massage — this can worsen inflammation.
If pumping, pump for 10–15 minutes, then hand express for 2 minutes afterward to remove as much milk as possible.
Step 2: Ice, Not Heat
This is where a lot of moms go wrong. Ice after feeding, not heat. Too much heat increases inflammation. Ice the affected area for 15 minutes after each session. You can use a warm compress briefly before nursing to support letdown, but ice is your friend here.
Step 3: Ibuprofen
Take ibuprofen 600–800mg every 6–8 hours for pain and inflammation. This is safe while breastfeeding and makes a significant difference in both comfort and recovery. Acetaminophen can help with fever but won't address the inflammation the way ibuprofen does.
Step 4: Rest. Seriously.
Treat your body like you have the flu — because you essentially do. If you have mastitis, regular life needs to stop as much as possible. Sleep, hydrate, and let other people handle everything else. This is not optional.
Step 5: Green Cabbage Leaf (For Severe Cases or While Waiting for Antibiotics)
This sounds old-fashioned but there's real evidence behind it. For significant swelling, pain, or while you're waiting to reach your provider:
Take a cooled green cabbage leaf and briefly dip it in boiling water for 1–2 minutes to soften it (this is called "flashing")
Let it cool for 5–10 seconds, then fold or roll it to fit the affected area
Wrap it against the breast in saran wrap or hold it in place with a soft cloth
Avoid the nipple and areola
Apply for 24–48 hours as needed, until swelling and redness begin to decrease
Step 6: Antibiotics — Don't Wait Too Long
If your symptoms haven't meaningfully improved within 12–24 hours of starting home treatment, call your OB, midwife, or primary care provider for an antibiotic. Common antibiotics prescribed for mastitis include dicloxacillin and cephalexin — both safe for breastfeeding.
Take the full course even if you start feeling better. If you're not improving within 2–3 days of starting antibiotics, call back — you may need a milk culture or a different antibiotic.
What NOT to Do With Mastitis or Clogged Ducts
These are some of the most common mistakes we see — and they can make things significantly worse:
Do NOT power pump — this over-stimulates the breast and can worsen inflammation and swelling
Do NOT use a vibrating massage tool — heat and vibration together increase inflammation
Do NOT apply heat for long periods — 15 minutes max before nursing; ice after
Do NOT stop breastfeeding — milk stasis is the enemy; keep things moving
Do NOT massage deeply or aggressively — gentle, front-to-back only
Do NOT wait it out if you have a fever — mastitis with fever needs prompt treatment
When to Call Your Doctor or IBCLC
Call your doctor promptly if:
You have a fever of 101°F or higher
You have flu-like symptoms — chills, body aches, extreme fatigue
Your symptoms aren't improving after 12–24 hours of home treatment
You develop a painful lump that feels soft in the center — this may be a breast abscess, which requires drainage
You see red streaks spreading from the affected area
Call or book with an IBCLC if:
You're getting recurrent clogged ducts (more than once)
You have a bleb that isn't resolving
You're not sure if it's a clog, engorgement, or mastitis
Your pump isn't draining the affected side well
You want to prevent this from happening again
Early support makes all the difference. Most clogged ducts can be resolved in one IBCLC visit. Most cases of mastitis, caught early and treated correctly, resolve within a few days without complications.
Frequently Asked Questions
How long does mastitis last? With prompt treatment — rest, ibuprofen, continued nursing, and antibiotics if needed — most cases of mastitis improve significantly within 2–3 days. Without treatment, mastitis can worsen quickly and may progress to a breast abscess, so don't wait.
Can I still breastfeed with mastitis? Yes — and you should. Continuing to nurse or pump is one of the most important parts of treatment. Milk from a breast with mastitis is safe for your baby.
Is mastitis contagious? No. Mastitis is not contagious. It's an inflammation of your breast tissue, not a condition that can spread to your baby or others.
What causes recurring mastitis? Recurring mastitis is usually a sign of an underlying issue — most often a latch problem, a flange that doesn't fit well, or incomplete breast emptying at feeds. An IBCLC can help identify the root cause and break the cycle.
Can mastitis go away on its own without antibiotics? Non-infectious mastitis sometimes resolves with rest and supportive care alone. However, if you have a fever and flu-like symptoms, you need antibiotics — don't try to wait it out. Untreated bacterial mastitis can develop into an abscess, which is much harder to treat.
Can I get mastitis if I'm not breastfeeding? Yes, though it's far less common. Non-lactational mastitis can occur and should be evaluated by a doctor.
How do I prevent mastitis from coming back? The key is consistent, complete breast emptying — which means a good latch, a properly fitted pump flange, and not going too long between feeds or pumping sessions. An IBCLC can do a full assessment and help you identify any gaps in your routine.
Get Support From a Lactation Loop IBCLC
Mastitis, clogged ducts, and engorgement are all treatable — and you don't have to figure them out alone at 2am. Our board-certified IBCLCs offer in-home and in-office visits across Florida, Michigan, Texas, New York, North Carolina, and Indiana, and most major insurance plans are accepted including Aetna, Cigna, UHC, Anthem, UMR, Meritain, Wildflower, Lactation Network, and Curative.
Book an appointment with a Lactation Loop IBCLC → lactationloop.com/services
Not sure if you need a visit? Call us at 941-254-2502 — we're happy to help you figure out next steps.
Related reading: How to Increase Milk Supply: What Actually Works (And What Doesn't) — lactationloop.com/blog/how-to-increase-milk-supply-what-actually-works-and-what-doesnt Complete Guide to Pumping — lactationloop.com/blog/all-about-pumping