The Complete Pumping Guide for New Moms — Everything Your IBCLC Wants You to Know
Whether you're planning to exclusively pump, combining nursing and pumping, building a freezer stash, or preparing to return to work — pumping is one of the most asked-about topics our IBCLCs cover every single day.
And no wonder. Between choosing a pump, figuring out flange sizes, decoding pumping schedules, and navigating the world of wearable pumps, it can feel overwhelming before you've even brought your baby home.
This guide cuts through the confusion. Consider it everything your IBCLC would tell you if you had an hour together — straight from our board-certified lactation consultants serving families across Michigan, Florida, Texas, New York, North Carolina, and Indiana.
If this overwhelms you, we highly recommend you meet with a consultant prenatally. Prenatal consult will help you navigate each area of the breastfeeding journey and customize the visit to you and your needs. For the fastest service text us @ 941-254-2502 to schedule.
First Things First — Do You Actually Need to Pump?
Not every breastfeeding mom needs to pump. If you're nursing exclusively, your baby is gaining weight well, and you have no plans to be separated from your baby, pumping may not be necessary in the early weeks.
That said, most families benefit from introducing pumping at some point — whether for flexibility, building a stash, returning to work, or protecting supply when nursing is difficult. The key is knowing when and how to introduce it without disrupting what's already working.
General IBCLC guidance:
● If nursing is going well, you may want to wait before introducing routine pumping.
● If you're separated from your baby, returning to work early, or have supply concerns, routine pumping should begin.
● If you plan to exclusively pump, begin as soon as possible after birth — ideally within the first few hours
Choosing the Right Breast Pump
Your pump matters more than most people realize. Here's a quick breakdown of your main options:
Hospital-Grade Pump This was the gold standard for establishing supply, especially in the early days. If you have a NICU baby, you may be offered one of these. They are helpful but not necessary and can be costly if you need to rent. With so many new double electric pumps on the market they are not necessary but can be helpful if your personal pump is not accessible.
Personal Electric Double Pump The most common choice for nursing moms prenatally and postpartum is Spectra. This is the most recommended brand among IBCLCs. Most are covered by insurance through the Affordable Care Act — contact your insurance before purchasing. Blue has a chargeable battery option. Pink needs to remain plugged in at all times. The motor quality on each is the same. The Gold and portable versions are okay, but not the number choice due to tech challenges. Other reputable favorite pumps are Motif, pumpables genie and lansinoh. Medela is not longer at the top of our list but can be used if thats your only option.
Wearable / Hands-Free Pump Brands like Eufy, Willow, Baby Buddha, Elvie, Pumpbables Genie and Momcozy have exploded in popularity — and for good reason. They allow you to pump discreetly while going about your day. However, wearable pumps can be difficult to navigate in the early days as the flange sizing is not a one size fits all, the construction of the pumps are not ideal during engorgement and the sizing is not easily viewed due to the engineering of the product. Therefore investing and or using these pumps are recommended once flange sizing and milk supply is established with a traditional double electric.
Manual Pump Useful in the early days, as a backup, during travel or power outages. Some mothers simply prefer them. The output and efficiency in many scenarios is better than a double electric. The only down side is the manual part. Use of the hand to pump the handle can be uncomfortable for some mothers and not as convenient when caring for children.
Our IBCLC tip: Insurance coverage varies. Always check your specific plan before purchasing, and ask your IBCLC which pump they recommend based on your individual situation — one size does not fit all.
The Most Important Thing Nobody Tells You — Flange Sizing
If there is one thing that makes the biggest difference in your pumping experience — and the one thing most moms get wrong — it is flange size.
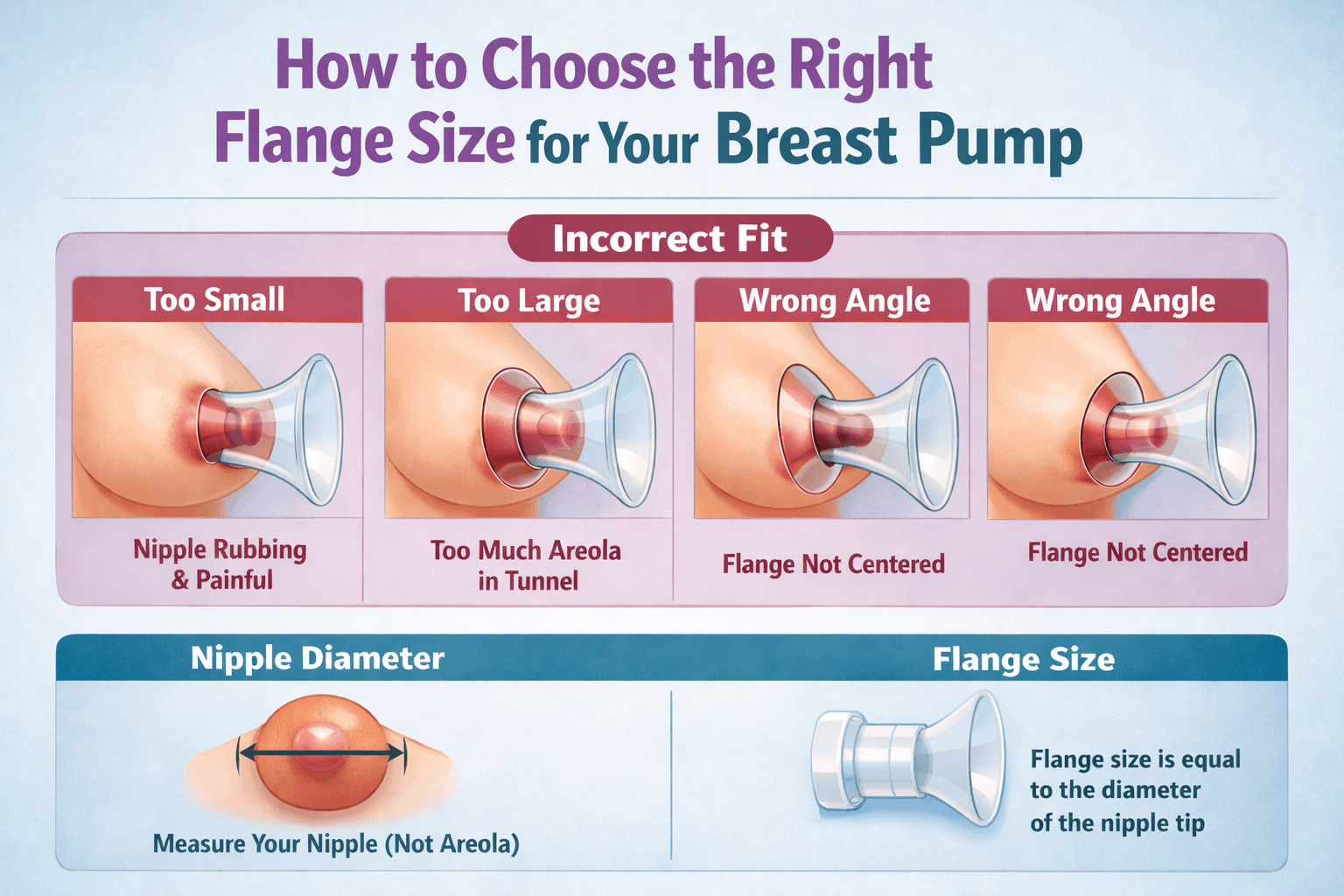
A flange (also called a breast shield) is the funnel-shaped piece that fits over your nipple. If it's the wrong size, pumping will be uncomfortable, inefficient, and can actually damage your nipple tissue and reduce your output over time.
Signs your flange is too large:
● Your areola is being pulled into the tunnel and it creates swelling
● You feel little to no suction sensation, this usually due to poor shape
● Output is low despite correct pump settings, the breast do not feel drained
● You continue to get mastitis, clogged ducts or blebs
Signs your flange is too small:
● Your nipple is rubbing against the sides of the tunnel creating pain
● Pumping is painful, pinchy or swollen
● Nipple appears white or blanched after pumping
● Restricted milk flow, poor milk removal
● Recurring mastitis, clogged ducts or blebs
The right fit: Your nipple should move freely in the tunnel with just a small amount of areola — no more than a few millimeters — being drawn in. The nipple is first and the areola moves behind it. There should be no friction, pinching, or pain. The tissue can touch the sides as long as its comfortable.
Flange sizing is not something you should guess at — and the size printed on your pump packaging is not necessarily your size. There are hundreds of products and flange shapes on the market. Each woman has a different shape, size and milk production. Therefore a professional pump fitting with an IBCLC takes the guesswork out completely and can transform your pumping experience overnight. Lactation Loop offers professional pump fittings at all of our locations across Michigan, Florida, Texas, New York, North Carolina, and Indiana.
Pumping Schedules — What Actually Works
There is no single pumping schedule that works for every mom. Your ideal schedule depends on your baby's age, whether you're also nursing, your supply goals, and your daily life. Here's a framework to start from:
Newborn stage (0–4 weeks) — if exclusively pumping:
● Pump 8–12 times in 24 hours- this varies based on the production
● Sessions every 2–3 hours, including at least one overnight session, often two.
● Each session 10–20 minutes, or until milk flow slows to drops. This range is based on the type of pump, production and if there are multiple babies involved.
● The overnight session (typically between 1–4am) is important — prolactin levels are highest then
Newborn stage — if nursing and pumping:
● Pump after nursing sessions, not instead of them
● Focus on one or two pumping sessions per day to begin building a stash
● Avoid over-pumping in the first weeks — too much stimulation can lead to oversupply
Once supply is established (4–12 weeks):
● Exclusive pumpers can begin to consolidate — dropping to 7–8 sessions per day
● Nursing + pumping moms can increase stash-building sessions as needed
● Morning pumps typically yield the most milk — prioritize them
Return to work:
● Pump as often as your baby would nurse — typically every 2–3 hours
● Be sure to keep core body temp warm during pumping, wear a sweater or jacket avoid cold vented areas when possible, drink warm drinks like hot tea.
● Pump both sides simultaneously for efficiency
● Keep a dedicated work pumping bag stocked and ready
Power Pumping — What It Is and When to Use It
Power pumping is a technique designed to mimic cluster feeding and signal your body to produce more milk. It is particularly useful if your supply has dropped or you want to boost output before returning to work.
A typical power pumping session:
● Pump 12 minutes
● Rest 10 minutes
● Pump 8 minutes
● Rest 15 minutes
● Pump 5 minutes
Do this once a day, for several days, ideally in the morning when prolactin levels are highest, or before bed when you are relaxed and done working for the day. Most moms notice a supply increase within 3–5 days of consistent power pumping.
Power pumping is not recommended as an everyday long-term strategy — it is best used as a targeted boost when you need it. If you are power pumping regularly without seeing results, reach out to your IBCLC. There may be an underlying supply issue that needs a more tailored approach.
Building a Freezer Stash — How Much Do You Actually Need?
The "perfect" freezer stash is a major source of anxiety for many new moms — and it doesn't need to be. Here's what our IBCLCs actually recommend:
If you're returning to work: You need enough milk to cover your baby's needs for 1–2 days before your supply catches up with the demand of pumping at work. That's typically 20–40 ounces — not the hundreds of bags some social media accounts suggest.
Storage guidelines:
● Room temperature: up to 4-8 hours; varies on location longer when at home
● Refrigerator: up to 4-8 days; may freeze at any time
● Freezer (standard): up to 6-12 months; depends on the quality of the freezer
● Deep freezer: 12-18 months also depends on the quality of storage and machine
Our IBCLC tip: Store milk in small amounts (2–4 ounces) to avoid waste. Babies' needs change and defrosted milk cannot be refrozen.
Wearable Pumps — The Honest Truth
Wearable pumps are genuinely life-changing for many moms — the freedom to pump while cooking, working, or chasing a toddler is real. But there are some important caveats:
What wearable pumps do well:
● Convenience and discretion
● Maintaining supply between traditional pump sessions
● Pumping on the go, at work, or during commutes
Where wearable pumps fall short:
● They typically don't empty the breast as completely as a traditional pump
● They are not ideal for establishing supply in the early weeks
● Flange sizing is important — and often harder to assess — in wearable pumps, otherwise one is at risk of having lowered output.
Our recommendation: Use a wearable pump as a supplement to, not a replacement for, your primary electric pump to start— especially in the first 6–8 weeks. Once supply is well established, many moms transition to using their wearable pump as their primary daytime pump with great success.
Returning to Work — Your Pumping Game Plan
Returning to work is one of the most common reasons moms reach out to Lactation Loop — and one of the most emotionally and logistically challenging transitions of early motherhood. Here's how to set yourself up for success:
2–4 weeks before your return:
● Begin building your stash with one morning pumping session daily
● Practice with your pump at home so the routine feels familiar
● Book a return-to-work pumping consultation with your IBCLC
Before your first day back:
● Know your rights — federal law requires employers to provide reasonable break time and a private space (not a bathroom) for pumping
● Set up your pumping station at work in advance
● Pack your pumping bag the night before
On the job:
● Pump every 2–3 hours — skipping sessions leads to supply drops
● Use a hands-free pumping bra to maximize efficiency
● Keep a photo or video of your baby on your phone — looking at your baby while pumping can increase oxytocin and improve output
● Stay hydrated and fed — your body cannot make milk without adequate calories and fluids
When supply drops after returning to work: This is extremely common and does not mean you have to stop breastfeeding. Add a pumping session in the evening, try power pumping on weekends, and contact your IBCLC — most supply dips after returning to work are very manageable with the right support.
When to Call Your IBCLC About Pumping
You don't have to be struggling to reach out to a lactation consultant. In fact, the best time to work with an IBCLC about pumping is before problems start. That said, definitely reach out if you're experiencing:
● Pumping output that seems low despite frequent sessions
● Pain or discomfort while pumping
● Nipple damage — cracking, bleeding, or blistering
● A sudden drop in supply
● Difficulty transitioning from nursing to pumping or vice versa
● Confusion about which pump to choose or how to use it
● Preparing to return to work and wanting a personalized plan
A professional pump fitting and pumping consultation with your IBCLC can resolve most pumping challenges quickly and get you back on track — covered by most major insurance plans.
Book a Pumping Consultation with Lactation Loop
Lactation Loop's board-certified IBCLCs offer professional pump fittings and personalized pumping consultations across all of our locations — in-home, in-office, and virtually statewide and internationally.
We accept most major insurance plans within the US including Aetna, Anthem, Cigna, UnitedHealthcare (UHC), UMR, Meritain, Wildflower and the Lactation Network. Many families find their visits are fully covered under the Affordable Care Act with no out-of-pocket cost.
Call or text us at 941-254-2502 or book online below. You've got this — and we've got you.
Lactation Loop is a collective of board-certified IBCLC lactation consultants serving families across Michigan, Florida, Texas, New York, North Carolina, and Indiana with in-home, in-office, and virtual lactation consultant visits. Most insurance accepted.